Deep Brain Stimulation: A Breakthrough for Movement Disorders
Living with a debilitating movement disorder can profoundly impact every aspect of life, from simple daily tasks to social interactions and overall independence. For many, the constant tremor, rigidity, or involuntary movements associated with conditions like Parkinson's disease, essential tremor, and dystonia can feel like an unending battle. While medications often provide initial relief, their effectiveness can wane over time, leaving patients searching for alternative solutions. This is where Deep Brain Stimulation (DBS) emerges as a powerful, life-changing treatment.
DBS is an innovative neurosurgical procedure that has revolutionized the management of several complex neurological conditions. Often described as a "pacemaker for the brain," it involves implanting tiny electrodes in specific areas of the brain that are responsible for controlling movement. These electrodes then deliver continuous, precisely controlled electrical impulses, effectively re-regulating abnormal brain activity that causes symptoms. For individuals whose lives have been significantly compromised by uncontrolled tremors and other movement-related issues, DBS offers a beacon of hope, often providing immediate and dramatic relief where other treatments have failed.
Understanding Deep Brain Stimulation: How It Works
At its core, Deep Brain Stimulation works by targeting the specific brain circuits that are malfunctioning and causing involuntary movements. Imagine your brain as an intricate network of electrical wires. In movement disorders, some of these wires might be short-circuiting or sending out chaotic signals, leading to symptoms like tremors or muscle rigidity. DBS acts like a sophisticated noise-cancellation system, interrupting and harmonizing these aberrant signals.
The process begins with the careful implantation of small, thin electrodes, known as leads, into precise areas deep within the brain. These areas are typically part of the basal ganglia, a group of structures critical for motor control. For example:
- For Essential Tremor, the thalamus is often targeted.
- For Parkinson's Disease, the subthalamic nucleus (STN) or globus pallidus interna (GPi) are common targets.
- For Dystonia, the globus pallidus interna (GPi) is frequently the focus.
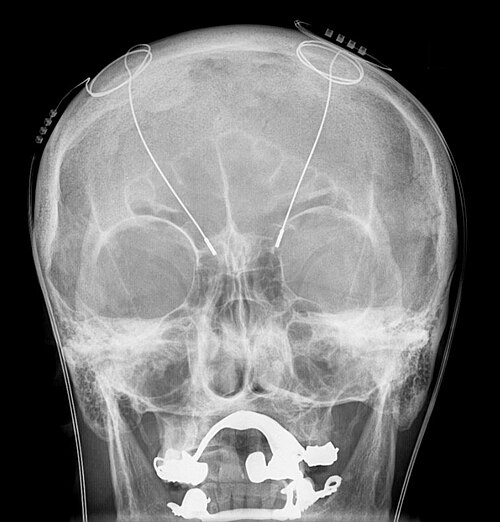
Once implanted, these electrodes are connected by thin wires that run discreetly underneath the skin, down the neck, and to a small, battery-operated device called an implantable pulse generator (IPG) – similar to a cardiac pacemaker. This IPG is typically placed under the skin in the chest, near the collarbone. Once activated, the IPG sends continuous, low-level electrical impulses through the wires to the electrodes in the brain. These impulses modulate the abnormal brain activity, helping to restore more normal function and significantly reduce symptoms.
The beauty of DBS lies in its adjustability. After the surgery, a neurologist or neurosurgeon specializing in DBS can program and fine-tune the settings of the IPG wirelessly, optimizing the electrical stimulation to maximize symptom control while minimizing potential side effects. This personalized approach means the treatment can be tailored to each patient's unique needs, often leading to profound improvements in quality of life.
Who Can Benefit: Conditions Treated by DBS
Deep Brain Stimulation is not a universal cure for all neurological ailments, but it has proven exceptionally effective for a select group of movement disorders, particularly when conventional medical therapies are no longer sufficient. If you're exploring this option, it's vital to consult with a movement disorder specialist to determine if you're a suitable candidate. For more detailed insights into its applications, consider reading DBS Treatment for Parkinson's, Essential Tremor & Dystonia.
The primary conditions for which DBS is currently approved and widely used include:
Essential Tremor
This is one of the most common movement disorders, characterized by involuntary, rhythmic shaking, most often in the hands and arms, but also affecting the head, voice, and legs. While not life-threatening, severe essential tremor can be profoundly disabling, making everyday tasks like eating, drinking, writing, or dressing nearly impossible. When medications fail to provide adequate relief, DBS can offer remarkable control over the tremor, often providing immediate and significant improvement post-activation. Patients frequently report regaining independence and confidence in performing daily activities they once found challenging.
Parkinson’s Disease
Parkinson's disease is a progressive neurological disorder that affects movement, balance, and coordination. Its core motor symptoms include tremor at rest, bradykinesia (slowness of movement), rigidity, and postural instability. While levodopa medication is highly effective for many, over time, its benefits can fluctuate, leading to "on-off" periods and dyskinesias (involuntary writhing movements) as side effects. DBS can significantly reduce these motor symptoms, lessen medication dependence, and smooth out motor fluctuations, leading to a more consistent "on" time and improved overall quality of life. It’s important to note that DBS primarily addresses motor symptoms and does not cure the disease or halt its progression.
Dystonia
Dystonia is a neurological disorder characterized by sustained or repetitive muscle contractions, resulting in twisting and repetitive movements or abnormal fixed postures. It can affect a single part of the body (focal dystonia) or be widespread (generalized dystonia). When medications like botulinum toxin injections or oral muscle relaxants are ineffective or cause intolerable side effects, DBS can be a highly effective treatment, particularly for generalized or segmental dystonia. It works by normalizing the abnormal signals that cause muscle spasms, leading to reduced involuntary movements and improved posture.
Other Disorders Causing Involuntary Tremors or Shaking
While less common, DBS may also be considered for other severe, medication-refractory movement disorders that cause debilitating tremors or involuntary movements, following thorough evaluation by a specialized medical team. This highlights the broad potential of neuromodulation to address a range of complex neurological challenges.
The DBS Journey: From Evaluation to Ongoing Care
Embarking on the Deep Brain Stimulation journey is a significant decision that involves several stages, from rigorous evaluation to the surgical procedure itself, and then ongoing post-operative care. It's not a quick fix but a carefully managed process designed to achieve the best possible outcome.
Candidacy and Pre-Procedure Evaluation
The first and most crucial step is a comprehensive evaluation to determine if you are a suitable candidate for DBS. This typically involves a multidisciplinary team, including a neurologist, neurosurgeon, neuropsychologist, and sometimes a psychiatrist or speech therapist. The criteria often include:
- Diagnosis of a DBS-responsive movement disorder (e.g., advanced Parkinson's, severe essential tremor, or dystonia).
- Symptoms that are significantly disabling and have not responded adequately to optimal medical therapy.
- Absence of severe cognitive impairment or psychiatric conditions that could complicate the procedure or recovery.
- Realistic expectations about the potential benefits and limitations of DBS.
- Good general health to tolerate surgery.
During this phase, you will undergo various tests, including detailed neurological exams, advanced brain imaging (MRI, CT), and sometimes a "levodopa challenge" for Parkinson's patients, to assess medication responsiveness. This meticulous evaluation ensures the procedure's safety and maximizes the chances of a successful outcome.
The Surgical Procedure
To implant the necessary equipment for Deep Brain Stimulation, skilled neurosurgeons utilize advanced brain mapping imaging technology to pinpoint the exact locations for electrode insertion. This precision is paramount, as even a millimeter can make a difference in effectiveness. Small holes are made in the skull, through which the electrodes are carefully inserted into the targeted brain regions. Depending on the patient's condition and the surgical team's protocol, patients may be awake during part of the procedure (to allow for real-time symptom assessment during electrode placement) or under general anesthesia.
Once the electrodes are in place, wires are routed underneath the skin of the scalp and neck, connecting to the battery pack (IPG) inserted underneath the skin in the chest. The procedure typically lasts several hours.
Post-Procedure and Programming
The surgery is just the beginning. The real therapeutic benefits often become apparent during the programming phase, which usually starts a few weeks after surgery to allow for healing. A neurologist or trained specialist will use a specialized device to wirelessly adjust the electrical stimulation parameters (e.g., voltage, pulse width, frequency) delivered by the IPG. This process is highly individualized and may require several programming sessions over weeks or months to find the optimal settings that provide the best symptom control with minimal side effects.
Patients are actively involved in this process, providing feedback on how the stimulation affects their symptoms. It's during this phase that many patients experience the most dramatic improvements, finding immediate relief from tremors or other involuntary movements once the system is correctly programmed.
Living with DBS and Ongoing Care
Once optimal settings are found, living with DBS becomes part of daily life. The IPG battery typically lasts 3-5 years (or longer for rechargeable systems) before needing replacement through a minor outpatient procedure. Regular follow-up appointments with your neurologist are essential to monitor your condition, make any necessary programming adjustments, and manage your medications. For practical tips on managing your condition and the role of DBS, you might find Deep Brain Stimulation: A Guide to Relieve Tremors helpful.
Benefits and Considerations of DBS
While Deep Brain Stimulation offers significant hope, it's important to have a balanced understanding of its potential benefits and the considerations involved.
Key Benefits
- Significant Symptom Control: DBS can dramatically reduce debilitating tremors, rigidity, bradykinesia, and dystonic spasms, often leading to immediate and sustained relief.
- Reduced Medication Dependency: Many patients can significantly lower their dosage of oral medications, thereby reducing troublesome side effects like dyskinesia in Parkinson's disease.
- Improved Quality of Life: By restoring motor function, DBS often leads to greater independence, improved ability to perform daily activities, enhanced social engagement, and a better overall sense of well-being.
- Reversible and Adjustable: Unlike some other surgical interventions, DBS is adjustable and reversible. The stimulation can be turned off, and parameters can be changed to adapt to disease progression or side effects.
Important Considerations and Potential Risks
- Surgical Risks: As with any brain surgery, there are inherent risks, though rare, including infection, bleeding (which could lead to stroke), or adverse reactions to anesthesia.
- Hardware-Related Issues: The DBS system components can sometimes malfunction. Electrodes might shift, wires could break, or the battery might fail prematurely, potentially requiring additional surgery.
- Programming Side Effects: While DBS aims to reduce symptoms, the electrical stimulation can sometimes cause temporary or adjustable side effects such as speech difficulties, balance problems, tingling sensations, or mood changes. These are usually manageable through programming adjustments.
- Not a Cure: DBS treats symptoms; it does not cure the underlying neurological condition or halt its progression.
- Ongoing Management: Living with DBS requires regular follow-up appointments for programming adjustments and battery management.
Choosing DBS is a highly personal decision made in close consultation with a specialized medical team, weighing the potential benefits against the risks for your specific situation.
Conclusion
Deep Brain Stimulation stands as a testament to the remarkable advancements in neurosurgery and neuromodulation, offering a transformative solution for individuals grappling with severe, medication-refractory movement disorders. By precisely targeting and re-regulating dysfunctional brain circuits, DBS can profoundly alleviate symptoms such as debilitating tremors, rigidity, and dystonic spasms, restoring a level of function and independence many thought lost. While it represents a significant medical undertaking, the potential for vastly improved quality of life, reduced medication burden, and renewed participation in daily activities makes DBS a truly groundbreaking therapy. For those whose lives are severely impacted by conditions like Parkinson's disease, essential tremor, or dystonia, exploring Deep Brain Stimulation with a qualified specialist could open the door to a future with greater control, comfort, and freedom.